Why is vulvodynia worse at night?
As a specialist dedicated to comprehensive women’s wellness, I, Dr. Jay Mehta, often hear a poignant and frustrating question from my patients:
“Why is the burning, stinging pain of vulvodynia so much worse once I settle down for the night?” It’s a common and highly challenging complaint for those suffering from this chronic condition.
The simple, yet complex, answer is that the worsening of vulvodynia symptoms at night is usually due to a perfect storm of neurological hypersensitivity, loss of distraction, and subtle physiological changes that occur when you transition from an active day to rest.
When you are busy, your brain filters out many pain signals; at night, that filter turns off, leaving the hyper-sensitized nerves of the vulva free to scream for attention.
Dealing with this kind of unprovoked, chronic discomfort requires more than just masking the symptoms; it demands a deep understanding and compassionate care, which is the cornerstone of the care we provide at Ahalya.

DR JAY MEHTA
Key Takeaways
- Vulvodynia is chronic, unexplained vulvar pain lasting over three months.
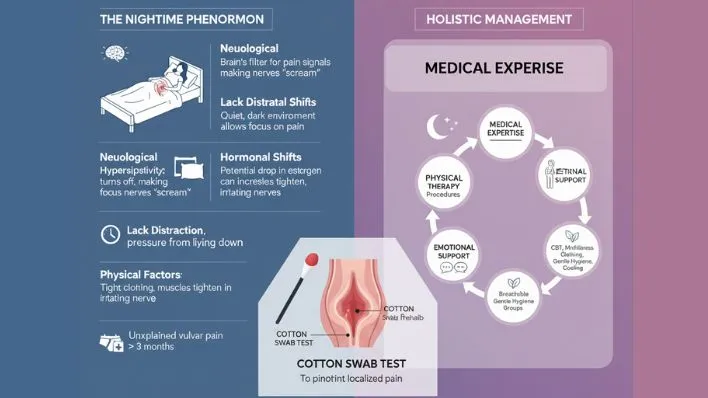
- The pain is often worse at night due to neurological hypersensitivity, hormonal shifts, lack of distraction, and physical factors like tight clothing or pressure in bed.
- Diagnosis is one of exclusion, often relying on the Cotton Swab Test to pinpoint localized pain.
- Effective treatment requires a comprehensive, multimodal approach combining topical medications, physical therapy (for pelvic floor dysfunction), nerve blocks, and emotional support.
- Seeking expert care is crucial for reducing chronic pain and improving quality of life.
TALK TO US
GET IN TOUCH ON
What exactly is vulvodynia?
Many people ask, “What is this mysterious pain down there?” Vulvodynia (pronounced vul-vo-DIN-ee-ah) is medically defined as chronic vulvar pain lasting at least three months without a clearly identifiable cause, such as an infection, skin disorder, or nerve entrapment.
The pain is typically described as a burning, stinging, raw, or throbbing sensation, which can range from mild annoyance to debilitating agony. The vulva is the external genital area, and vulvodynia essentially means “painful vulva.”
This condition is a pain syndrome, meaning the problem lies in how the nerves of the vulva are signaling pain to the brain, even when there is no visible injury or infection.
Why does the pain feel worse at night?
For many women, the heightened nocturnal discomfort is a primary hurdle to getting restorative sleep. This phenomenon, sometimes called “nocturnal vulval pain,” is rooted in several interconnected physical and psychological factors.
First, pain perception is highly subjective, and the lack of cognitive distraction in a quiet, dark room allows the brain to fully focus on the nerve signals.
Secondly, stress, which is often subconsciously processed throughout the day, causes the pelvic floor muscles—a hammock-like group of muscles supporting the pelvic organs—to tighten reflexively.
This constant muscle tension can irritate the hypersensitive pudendal nerve, exacerbating the burning sensation.
Furthermore, wearing tight nightwear or even the pressure of lying down in certain positions can create localized pressure on the vulvar vestibule (the opening of the vagina), which acts as a direct trigger for pain flare-ups.
What are the root causes of this chronic discomfort?
While the precise cause of vulvodynia remains unknown—which is why it is often called a diagnosis of exclusion—trusted medical research points toward a multifactorial etiology, or multiple factors working together.
The leading theories center on neuropathic pain, where the nerves supplying the vulva (especially the nerve endings) become damaged, irritated, or over-dense, leading to a state of constant hypersensitivity.
Other potential causes include chronic inflammation from previous severe infections (like yeast or UTI), hormonal imbalances (particularly a drop in estrogen), genetic factors that predispose some women to higher inflammatory responses, and dysfunction of the pelvic floor muscles (weakness or chronic spasm).
How do doctors classify vulvodynia?
When you consult a specialist, we classify the condition to tailor the treatment plan. The two main types are based on location and trigger:
- Localized Vulvodynia (Vestibulodynia): The pain is confined to one specific area, usually the vulvar vestibule. It is typically provoked—meaning it’s triggered by touch or pressure, such as during sexual intercourse, tampon insertion, or sitting.
- Generalized Vulvodynia: The pain occurs across different areas of the vulva and is often unprovoked (spontaneous), though pressure or touch may intensify it.
It’s important to understand that vulvodynia is not an STD and does not have physical “stages” like a progressive disease. It is a chronic pain condition that can be managed effectively with the right support.
How is a vulvodynia diagnosis confirmed?
The diagnosis of vulvodynia is primarily one of exclusion, which means we first rule out all other possible causes of vulvar pain.
This often involves a thorough physical exam, taking swabs to check for infections like thrush or bacterial vaginosis, and sometimes a biopsy to exclude inflammatory skin conditions.
The most defining test is the Cotton Swab Test (or point-pressure test), where a moistened cotton swab is gently used to apply pressure to specific areas of the vulva.
If this light touch elicits disproportionately severe, burning pain in the absence of visible physical findings, it strongly suggests vulvodynia.
This comprehensive approach is standard at leading cosmetic gynecology and wellness hospitals in Mumbai that focus on intimate health.
What are the most effective treatments available?
Because vulvodynia has multiple potential root causes, the most successful treatment is always a multimodal approach—combining several therapies personalized for the patient. This may include:
- Topical Medications: Applying local anesthetics (like lidocaine ointment) to numb the area, or prescription compounded creams that address nerve sensitivity or hormonal deficiencies.
- Oral Neuromodulators: Medications typically used to treat nerve pain (such as low-dose tricyclic antidepressants or anticonvulsants) are utilized to stabilize the overactive nerve signals, not to treat depression.
- Pelvic Floor Physical Therapy: Crucial for relaxing the tight and spasming pelvic floor muscles, which often contribute significantly to the pain cycle.
- Nerve Blocks or Injections: Injecting local anesthetics or other compounds near the affected nerves for targeted, longer-lasting relief.
- Procedural Treatments: In localized cases unresponsive to conservative methods, procedures like Vestibulectomy (surgical removal of the painful tissue) or the use of specific therapeutic lasers may be considered.
We offer advanced cosmetic gynecology treatments in Mumbai, ensuring patients have access to the full spectrum of modern pain management techniques.
How can I cope with the stress and emotional toll?
Living with chronic pain is exhausting and can lead to significant emotional distress, including anxiety, depression, and difficulties with intimacy.
We recognize that emotional care is a core component of recovery. Cognitive Behavioral Therapy (CBT) and mindfulness techniques can help you re-wire your brain’s response to pain signals, reducing the pain-anxiety cycle.
Finding a supportive, specialized therapist or joining a support group can significantly improve coping strategies and overall well-being.
This is not “all in your head”; it is a real neurological condition, and managing the emotional consequences is a sign of strength and self-care.
What lifestyle steps help prevent flare-ups?
Preventive awareness focuses on minimizing nerve irritation. I recommend the following:
- Wear breathable clothing: Opt for loose-fitting garments and 100% cotton underwear during the day, and consider sleeping without underwear at night.
- Use gentle hygiene: Avoid harsh, scented soaps, bubble baths, douches, and aggressive washing. Use a mild soap substitute or just warm water.
- Cooling and Protection: Use a cold pack wrapped in a soft cloth for acute flare-ups. Apply a protective barrier like plain petroleum jelly before swimming.
- Minimize pressure: Use a donut or foam cushion if you must sit for long periods. Avoid activities that create friction, like prolonged cycling or horseback riding, during flare-ups.
Frequently Asked Questions (FAQs)
1. Can dietary changes help with vulvodynia symptoms?
Some women find relief by reducing foods high in oxalates (like spinach, nuts, and chocolate), as these compounds might irritate the sensitive vulvar tissue in some individuals, though scientific evidence varies.
2. Is vulvodynia contagious?
Absolutely not. Vulvodynia is a chronic pain condition rooted in nerve dysfunction and inflammation, not an infection. It cannot be transmitted to a sexual partner.
3. Can menopause or hormonal birth control trigger vulvodynia?
Yes, hormonal fluctuations, particularly a drop in estrogen (which happens during menopause, or sometimes with certain birth control pills), can thin the vulvar tissue and increase nerve sensitivity, potentially leading to or exacerbating vulvodynia.
4. How is vulvodynia related to Interstitial Cystitis (IC) or Irritable Bowel Syndrome (IBS)?
Vulvodynia is often categorized alongside other chronic pain syndromes, like IC and IBS. These conditions share a common link through central nervous system sensitization, meaning if you have one, you are statistically more likely to have another.
5. Will the pain ever completely go away?
While vulvodynia is chronic, the goal of modern, expert treatment is remission, meaning reducing the pain to a manageable, non-bothersome level or achieving full resolution. Many women experience significant long-term relief with the correct multimodal therapy.
Conclusion
Vulvodynia is a challenging condition, but it is treatable. The nighttime aggravation is a clear sign that your body’s nervous system is stressed and hyperactive.
By understanding the neuropathic mechanisms and employing a comprehensive, individualized treatment plan—combining medical expertise with physical and emotional support.
We can successfully decrease the intensity of the burning, restore function, and significantly enhance your quality of life. Don’t resign yourself to living with this chronic discomfort. Take control of your health today.
If the persistent, burning pain of vulvodynia is disrupting your sleep and daily life, it’s time to seek specialized, compassionate care. Dr. Jay Mehta and the dedicated team at Ahalya Cosmetic Gynecology & Intimate Medicine Clinic in Mumbai understand the complexities of this condition.
Related Blogs
Hormonal Treatment for Perineal Endometriosis: GnRH, Progestins and the Pill
Perineal endometriosis doesn’t directly cause infertility. But coexisting pelvic disease can. Know what to check before trying to conceive. Expert care in Mumbai.
Surgical Treatment for Perineal Endometriosis: Wide Excision Explained
Wide local excision is the only proven cure for perineal endometriosis. Learn the procedure, recovery & recurrence prevention. Expert surgery in Mumbai.
How Is Perineal Endometriosis Diagnosed? MRI, Ultrasound and Biopsy Explained
Perineal endometriosis is diagnosed via clinical exam, ultrasound, MRI & biopsy. Know what each test involves & get expert diagnosis in Mumbai.
Symptoms of Perineal Endometriosis: Cyclic Pain, Nodules and What to Look For
Cyclic pain or a lump near your perineum that worsens during periods? It could be perineal endometriosis. Get expert diagnosis in Mumbai.
Perineal Endometriosis Causes and Risk Factors: Episiotomy, C-Section and More
Painful lump near episiotomy or C-section scar? It could be perineal endometriosis. Learn causes, symptoms & treatment. Expert care in Mumbai.
What Is Perineal Endometriosis? A Simple Explanation
Perineal endometriosis causes cyclical pain near episiotomy scars. Often misdiagnosed — get expert diagnosis & treatment at Ahalya Gynecology, Mumbai.
Pregnancy & Vaginismus: What Every Woman Should Know
Vaginismus doesn’t cause infertility — pregnancy is possible naturally or via IUI/IVF. Expert care at Ahalya Cosmetic Gynecology, Mumbai.
Vaginismus: Causes, Symptoms, Diagnosis & Treatment
Vaginismus causes involuntary muscle spasms, making penetration painful. Learn about symptoms, diagnosis, and effective treatments including physiotherapy and Botox.
Recurring UTIs After Sex: Causes, Prevention, and When to Worry
Sex moves bacteria toward your urethra, causing UTIs. Urinate after sex, stay hydrated & see a specialist if infections recur 3+ times a year.
Pelvic Floor Therapy Costs & Affordable Options for Teens
Pelvic floor therapy in Mumbai. Affordable teen options include virtual care & home programmes. Expert help at Ahalya Cosmetic Gynecology.
Book Appointment