Applying Vaginal Estrogen: A Simple Guide for Beginners
In my 13+ years of medical practice, I have seen countless women suffer silently with intimate discomfort, often unaware that a simple, localised treatment could dramatically improve their quality of life.
Vaginal estrogen is one of the most misunderstood yet effective therapies we have in women’s health.
Whether you are navigating menopause or recovering from postpartum changes, understanding how to use this medication correctly is the first step toward relief.
This guide is designed to walk you through the process safely, ensuring you feel confident and supported in your care.

DR JAY MEHTA
Key Takeaways
- Vaginal estrogen is a localised treatment that restores tissue health with minimal absorption into the bloodstream.
- Proper application ensures maximum effectiveness and reduces mess or discomfort.
- Consistency is key; symptoms often improve significantly within a few weeks of regular use.
- Always wash your hands and any reusable applicators thoroughly to maintain hygiene.
TALK TO US
GET IN TOUCH ON
Why have I been prescribed vaginal estrogen?
Many of my patients at Ahalya Cosmetic Gynecology in Mumbai initially feel hesitant about using hormone-based treatments. It is important to understand that unlike oral hormone replacement therapy (HRT), vaginal estrogen is a localised therapy.
This means it works directly on the vaginal tissues rather than circulating through your entire body. We typically prescribe it as a targeted
According to clinical data, vaginal estrogen is 80–90% effective in relieving symptoms of vaginal atrophy, such as dryness and discomfort, making it the gold standard for restoring intimate comfort.
Understanding the Benefits
- Restores Elasticity: It helps thicken the vaginal lining.
- Improves Lubrication: It increases natural moisture, reducing painful friction.
- Balances pH: It helps maintain a healthy acidic environment, reducing infection risks.
Is it messy or difficult to apply the cream or tablet?
This is the most common question I hear in the clinic. The short answer is no—once you know the technique, it is quick and simple.
Most vaginal estrogen comes in one of three forms: a cream, a tablet (pessary), or a ring. While the ring is inserted and left in place for months, creams and tablets require regular application.
Preparation
- Hygiene First: Always wash your hands thoroughly with soap and water before starting.
- Timing Matters: I usually recommend applying the medication at bedtime. This allows the treatment to stay in place and be absorbed while you sleep, preventing leakage.
- Get Comfortable: You do not need to be in a clinical position. Lying on your back with knees bent or standing with one leg raised (like on a stool) works best.
How do I use the applicator correctly for cream?
If you have been prescribed estrogen cream, it usually comes with a reusable plastic applicator. Precision is helpful here to ensure you get the right dose without overfilling.
Step-by-Step Application
- Load the Applicator: Screw the nozzle of the applicator onto the tube of cream. Gently squeeze the tube until the plunger rises to the mark indicated for your prescribed dose (usually 0.5g or 1g).
- Insert Gently: Hold the applicator like a syringe. Relax your pelvic muscles. Gently insert the applicator into the vagina as far as it will comfortably go. Do not force it.
- Release the Cream: Slowly press the plunger down to release the cream into the vagina.
- Remove and Clean: Withdraw the applicator. Pull the plunger out of the barrel and wash both parts with warm, soapy water. Let them air dry.
Doctor’s Tip: If you find insertion uncomfortable due to dryness, you can put a tiny amount of the cream on the tip of the applicator to act as a lubricant.
What if I have been prescribed a vaginal tablet instead?
Vaginal tablets (often called pessaries) are small and less messy than creams. They usually come in a pre-loaded disposable applicator, which makes them very convenient for many of our patients.
Insertion Guide
- Check the Pack: Remove the applicator from the packaging. The tablet should already be seated at the end.
- Position and Insert: adopt the same comfortable position as above. Gently guide the applicator into the vagina until you feel slight resistance.
- Deploy the Tablet: Press the button or plunger on the end of the applicator to release the tablet.
- Disposal: Unlike cream applicators, tablet applicators are usually single-use. Dispose of the empty applicator in the bin.
The tablet will adhere to the vaginal wall and dissolve slowly overnight. You likely won’t feel it once it is inside.
How long will it take before I feel better?
Patience is essential here. While some women feel relief within a few days, it typically takes 2 to 3 weeks of consistent use to notice a significant reduction in dryness or irritation.
The Typical Treatment Schedule
- Loading Phase: Usually, you will apply the treatment every night for the first two weeks.
- Maintenance Phase: After the initial period, we often reduce the frequency to twice a week (e.g., Monday and Thursday nights) to maintain the benefits.
Do not stop abruptly just because you feel better. The symptoms of atrophy often return if the local estrogen support is removed completely.
Is it safe to have sex while using this medication?
Yes, absolutely. In fact, restoring intimate health is often the primary goal of this treatment. However, there are a few practical considerations to keep in mind.
Timing is Everything
If you plan to be intimate, do not apply the medication beforehand. It is best to apply your cream or tablet after sexual activity, right before you go to sleep.
Important Note regarding contraception: Some creams and oil-based capsules can weaken latex condoms and diaphragms. If you rely on barrier contraception, please discuss this with us so we can recommend safe alternatives or compatible products.
When should I worry about side effects?
Because the estrogen is concentrated in the vaginal tissue and very little enters the bloodstream, systemic side effects (like those associated with oral HRT) are extremely rare. Even so, the most common question I encounter is, “
However, you might experience mild local reactions initially, such as:
- Slight itching or irritation
- Mild vaginal discharge
- Spotting (very rare)
These usually subside as the tissue heals. If you experience heavy bleeding, severe pain, or breast tenderness, please contact your healthcare provider immediately.
Are you experiencing persistent discomfort or have questions about your intimate health?
At Ahalya Cosmetic Gynecology, we specialise in helping women regain confidence and comfort. We invite you to schedule a consultation with
Frequently Asked Questions (FAQs)
1. What is the recovery time after treatment for GSM?
Recovery time varies depending on the specific treatment chosen. Many patients experience improvements within a few weeks, but it is best to follow Dr. Jay Mehta’s advice and post-treatment care instructions for optimal results.
2. Are the treatments for GSM painful?
Most treatments are designed to be minimally invasive and cause little to no discomfort. Dr. Jay Mehta and the team at Ahalya Cosmetic Gynaecology prioritise patient comfort throughout the process.
3. Is GSM treatment suitable for menopausal women?
Yes, treatments for GSM are particularly effective for menopausal women who often experience symptoms due to hormonal changes. Options like hormonal therapy or laser treatments can be tailored to meet individual needs.
4. Will I need multiple treatment sessions for GSM?
Some treatments may require multiple sessions to achieve the desired results. During your consultation, Dr. Jay Mehta will provide a customised plan outlining the recommended number of sessions.
5. Are the treatments safe for women with pre-existing medical conditions?
Dr. Jay Mehta and the team ensure a thorough medical review before recommending any treatment to ensure it is safe and suitable for you, even if you have pre-existing medical conditions.
Conclusion
Taking charge of your intimate health is a powerful step. Vaginal estrogen is a safe, effective tool that has helped thousands of women reclaim comfort and intimacy.
By following these simple steps and sticking to your routine, you can manage symptoms effectively. Remember, we are here to support you through every stage of this journey.
Related Blogs
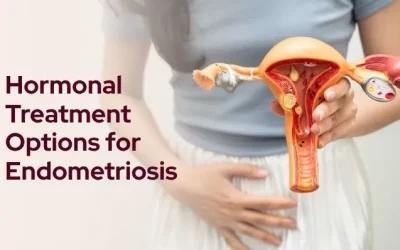
Hormonal Treatment for Perineal Endometriosis: GnRH, Progestins and the Pill
Perineal endometriosis doesn’t directly cause infertility. But coexisting pelvic disease can. Know what to check before trying to conceive. Expert care in Mumbai.
Surgical Treatment for Perineal Endometriosis: Wide Excision Explained
Wide local excision is the only proven cure for perineal endometriosis. Learn the procedure, recovery & recurrence prevention. Expert surgery in Mumbai.
How Is Perineal Endometriosis Diagnosed? MRI, Ultrasound and Biopsy Explained
Perineal endometriosis is diagnosed via clinical exam, ultrasound, MRI & biopsy. Know what each test involves & get expert diagnosis in Mumbai.
Symptoms of Perineal Endometriosis: Cyclic Pain, Nodules and What to Look For
Cyclic pain or a lump near your perineum that worsens during periods? It could be perineal endometriosis. Get expert diagnosis in Mumbai.
Perineal Endometriosis Causes and Risk Factors: Episiotomy, C-Section and More
Painful lump near episiotomy or C-section scar? It could be perineal endometriosis. Learn causes, symptoms & treatment. Expert care in Mumbai.
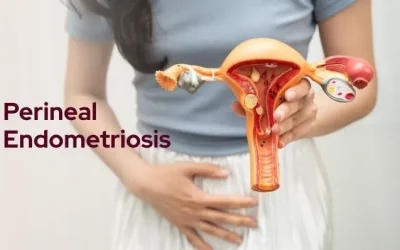
What Is Perineal Endometriosis? A Simple Explanation
Perineal endometriosis causes cyclical pain near episiotomy scars. Often misdiagnosed — get expert diagnosis & treatment at Ahalya Gynecology, Mumbai.
Pregnancy & Vaginismus: What Every Woman Should Know
Vaginismus doesn’t cause infertility — pregnancy is possible naturally or via IUI/IVF. Expert care at Ahalya Cosmetic Gynecology, Mumbai.
Vaginismus: Causes, Symptoms, Diagnosis & Treatment
Vaginismus causes involuntary muscle spasms, making penetration painful. Learn about symptoms, diagnosis, and effective treatments including physiotherapy and Botox.
Recurring UTIs After Sex: Causes, Prevention, and When to Worry
Sex moves bacteria toward your urethra, causing UTIs. Urinate after sex, stay hydrated & see a specialist if infections recur 3+ times a year.
Pelvic Floor Therapy Costs & Affordable Options for Teens
Pelvic floor therapy in Mumbai. Affordable teen options include virtual care & home programmes. Expert help at Ahalya Cosmetic Gynecology.
Book Appointment